Antiretroviral therapy has made it possible for people with HIV to live longer and healthier lives. However, in 2021, new vaccine technologies took center stage in regard to coronavirus infections, reminding those who have been affected by HIV/AIDS that a vaccine has yet to be developed for the human immunodeficiency virus.
HIV in the US today
With no known cure or prevention strategies beyond PrEP treatment, HIV infections have remained widespread in the United States year after year.
The CDC stated that in 2019 approximately 36,800 people received an HIV diagnosis in the US and its dependent areas. While these numbers indicate a great deal of progress made since the epidemic of the mid-1980s – when national rates were as high as 130,000 new cases per year – progress toward a vaccine has barely inched forward in the last 40 years.
HIV is also known to disproportionately affect the LGBTQ+ community and communities of color, with Black Gay and Bisexual men experiencing the majority of new cases each year, followed by Hispanic and Latino men.
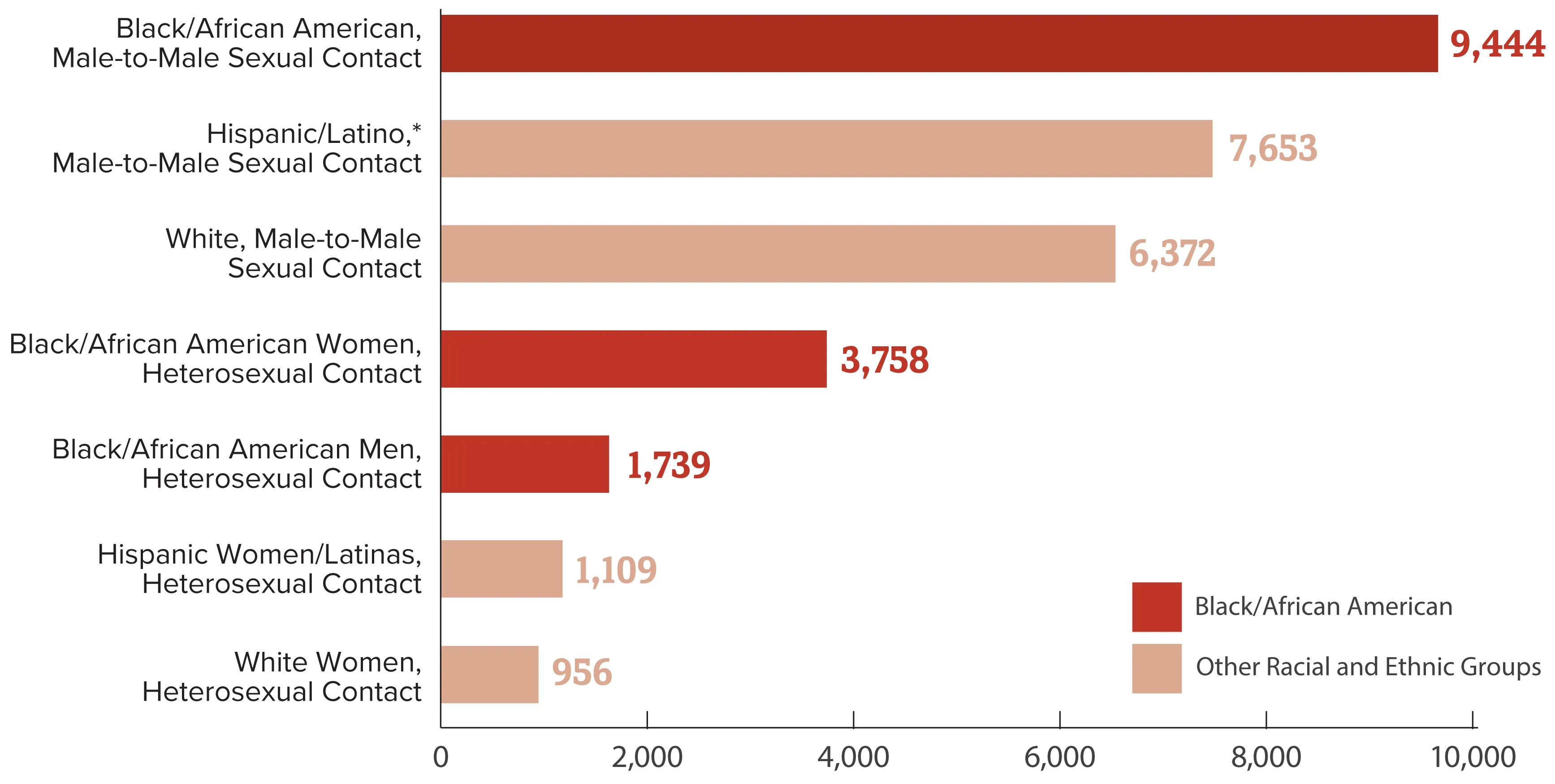
"Social and structural issues – such as HIV stigma, homophobia, discrimination, poverty, and limited access to high-quality health care – influence health outcomes and continue to drive inequities," according to the Centers for Disease Control.
Currently, the newest promising innovations for HIV vaccines, however exciting, are only being trialed as an aftereffect of coronavirus vaccine technologies. HIV has mutated innumerable times over the years, but now household-name companies are seeking to bring this new tech to the table in light of recent approval for the coronavirus.
Emergency use authorization of mRNA vaccines
Moderna and Pfizer BioNTech have launched a new era of medical technology with their mRNA coronavirus vaccines, swiftly approved for emergency use by the FDA.
HIV/AIDS activists have a long history of fighting for expedited approvals like this, as seen with the accelerated FDA approval of saquinavir for HIV treatment, announced in 1995 by Dr. Anthony Fauci (déjà vu, anyone?). This response only came after years of protests and organizing against the government's initial slow response to the crisis.
While mRNA technology was approved quickly due to the new pandemic, decades of HIV/AIDS research helped to inform the process, according to Stacey Hannah, director of research engagement at AVAC.
Since the emergency-use approval of mRNA vaccines last December, the FDA has gone on to fully approve both Moderna and Pfizer's vaccines. Now that the previously conceptual technology is proving effective, Moderna has taken the first steps in developing an HIV vaccine using mRNA.
In collaboration with the International AIDS Vaccine Initiative (IAVI) and the Bill and Melinda Gates Foundation (BMGF), candidate "mRNA-1644" is the first mRNA HIV vaccine to be trialed in humans. Researchers are hopeful that this new approach to development of an HIV vaccine will yield positive outcomes, especially after the recent failure of Johnson & Johnson's HIV vaccine in human trials.
Phase 1 of Moderna's study is scheduled to be completed in the spring of 2023. In the meantime, two other vaccines remain in human trials, with similar timelines. Mosaico and PrEPVacc are two large-scale trials ongoing around the world.
December 1 is World AIDS Day, and this year's theme in the US is "Ending the HIV Epidemic: Equitable Access, Everyone's Voice." While this is symbolic of hope and progress, HIV has persisted globally for the past 40 years and a vaccine is long overdue. However, new technologies like mRNA vaccines promise to offer new insights and potentially final products by 2023.